Cognitive Behavioral Therapy for Anxious Attachment: How CBT Helps You Build More Secure Relationships
Cognitive Behavioral Therapy for Anxious Attachment helps you manage fear of abandonment, overthinking, and reassurance-seeking in relationships. It works by changing unhealthy thought patterns and reactions, so you can build emotional stability, stronger boundaries, and more secure connections.
You know the feeling. A text goes unanswered. A plan changes. A partner sounds distant for one evening, and your mind starts writing a disaster story before the facts are even clear. For someone with anxious attachment, small moments can feel huge. They hit fast, stir fear, and push you toward checking, overexplaining, people-pleasing, or asking for reassurance again and again.
Cognitive Behavioral Therapy for Anxious Attachment can help, but not in the vague way many articles claim. It does not erase your history overnight, and it does not turn you into a different person. What it does is more useful. It teaches you how to spot the thoughts, body signals, and habits that keep relationship anxiety alive, then replace them with steadier responses you can actually use in daily life. CBT is a structured, goal-oriented form of therapy, and anxious attachment is strongly linked with lower self-esteem, fear of abandonment, and higher distress across mental health outcomes.
What anxious attachment really looks like in adult relationships
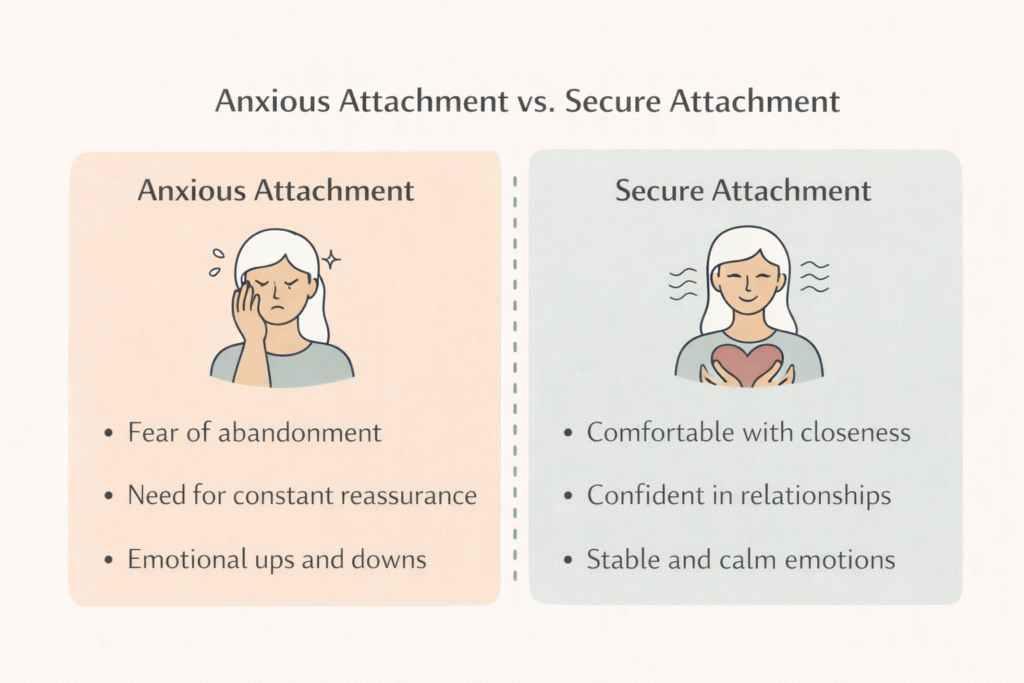
Anxious attachment is a pattern of relating marked by fear of rejection, fear of abandonment, and a heavy pull toward outside validation. You may read neutral behavior as a threat. You may feel unsteady when you are alone. You may trust your fear faster than you trust the relationship itself. Adults with this pattern often struggle with self-worth, sensitivity to criticism, jealousy, difficulty relaxing between contacts, and a strong need for reassurance. That does not mean you are irrational all the time. It means your system is primed to scan for distance and react fast.
This pattern often traces back to inconsistent early care, though adulthood experiences can keep it going. What matters now is not forcing a perfect story about childhood. What matters is understanding the loop that runs in the present. You notice a trigger. You assign meaning to it. Your body goes on alert. Then you do something to reduce the distress right now, even if that behavior makes things worse later. That is the loop CBT targets. It treats the thinking and behavior patterns that keep attachment anxiety active, instead of leaving you stuck at the level of insight alone.
Why CBT fits anxious attachment so well
CBT works well here because anxious attachment is not only emotional. It is also cognitive and behavioral. The pattern is fed by automatic thoughts such as “They are losing interest,” “I am too much,” or “If I do not fix this now, I will be abandoned.” Those thoughts drive behaviors like repeated texting, checking social media, overexplaining, testing the relationship, apologizing too much, or collapsing your own boundaries to keep closeness.
CBT was built for exactly this type of cycle. It helps you identify distorted thinking, examine evidence, test assumptions, and reduce unhelpful coping habits. It also gives you a framework for building new habits, not just discussing old pain. That matters because people with anxious attachment often understand their pattern intellectually but still react the same way when they are triggered. CBT narrows that gap between insight and action. It is also usually delivered over a limited course, often over a few months, though the timeline varies by person and problem severity.
There is one nuance most ranking pages skip. The evidence does not support the lazy claim that there is one universal CBT protocol made only for anxious attachment. What the evidence shows is more careful than that. CBT is well supported for anxiety-related problems, and some studies found that attachment anxiety improved during CBT in patients treated for panic disorder and social anxiety. That is promising, but it is not the same as saying every case of anxious attachment should be treated the same way. Good therapy adjusts the tools to the person in front of you.
The anxious attachment cycle CBT is trying to break
At the center of this issue is a loop that feels protective in the moment but keeps you trapped over time. It often looks like this:
- Trigger such as delayed replies, a change in tone, canceled plans, or physical distance
- Automatic thought such as “I did something wrong” or “They are pulling away”
- Body alarm such as tight chest, racing thoughts, stomach drop, restlessness
- Protective behavior such as checking, texting, pursuing, apologizing, pleasing, or withdrawing in protest
- Short relief, long-term cost because the relationship feels less stable, and your fear gets rewarded
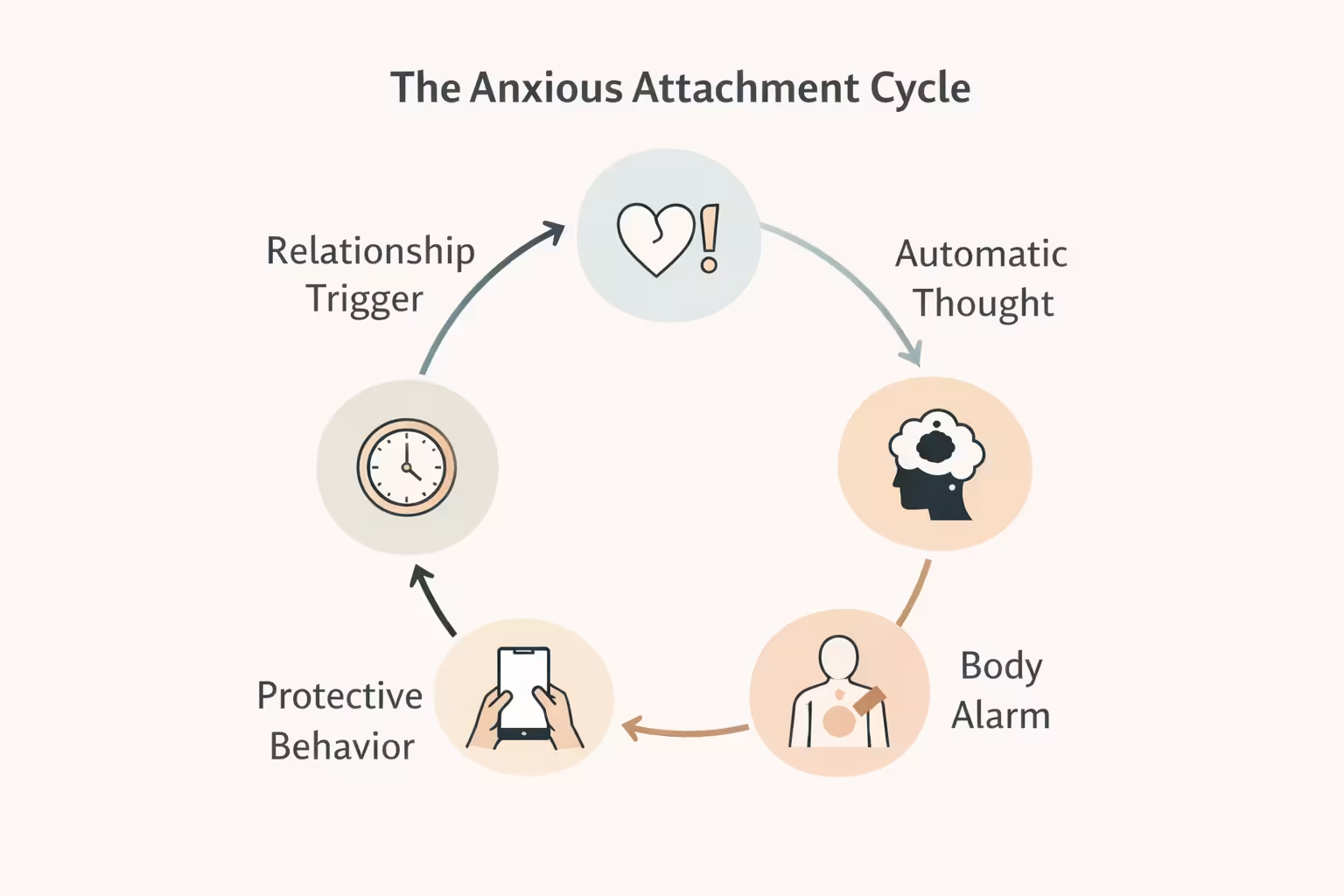
This cycle is brutal because reassurance can calm you briefly without fixing the real belief underneath. In fact, anxious attachment is strongly tied to excessive reassurance seeking, and research suggests that repeated reassurance seeking can fail to restore trust and may keep insecurity active. That is why CBT does not stop at “communicate better.” Sometimes better communication is needed. Sometimes the real work is learning not to obey every alarm your mind sends.
What happens in CBT for attachment anxiety
A solid course of Cognitive Behavioral Therapy for Anxious Attachment usually starts with assessment and pattern mapping. Your therapist will ask where the pattern shows up, what situations trigger it, what you think in those moments, how your body reacts, and what you do next. The goal is not to judge you. The goal is to make the invisible sequence visible. Once that sequence is clear, therapy becomes much more precise.
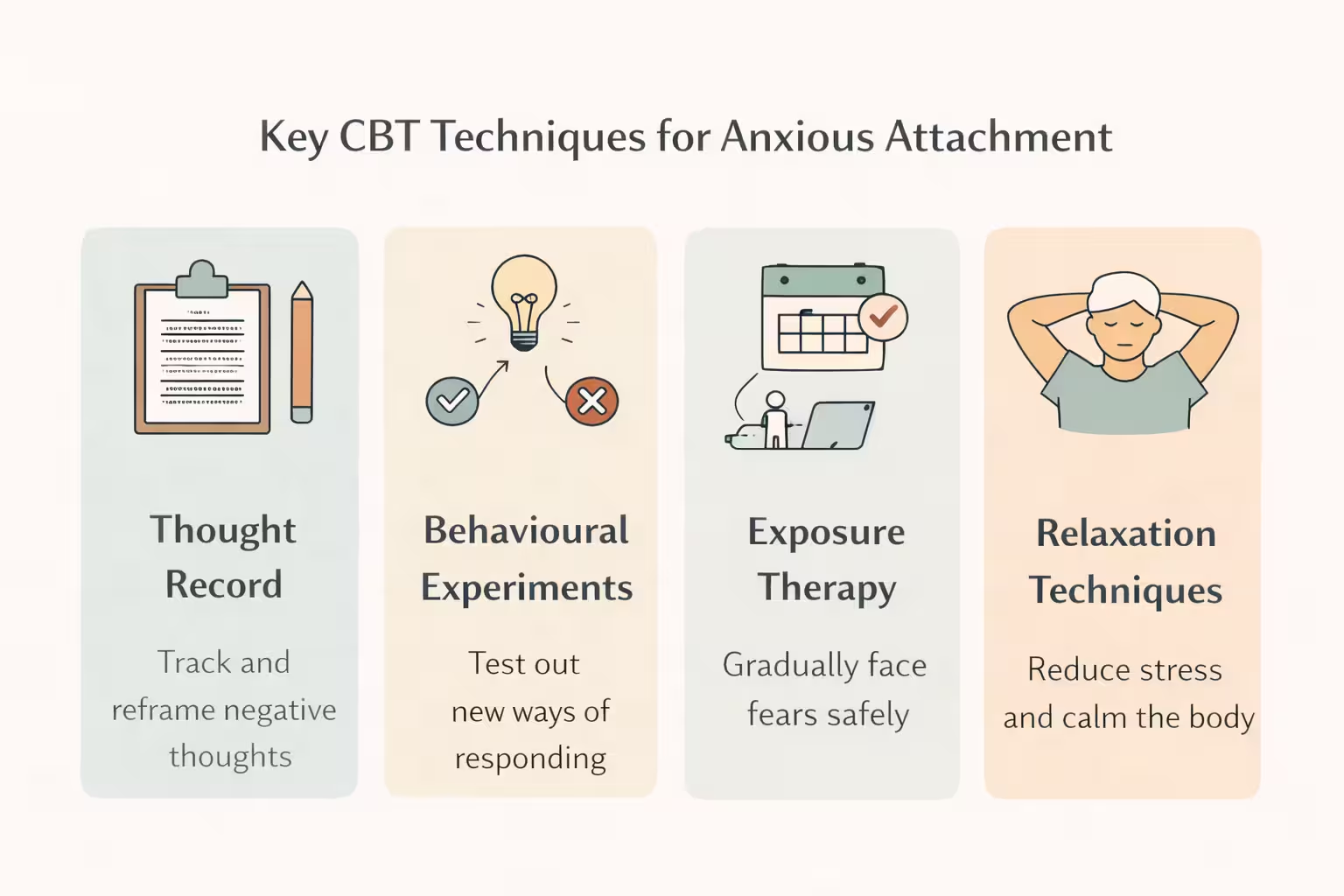
From there, CBT often focuses on five core tools. The first is cognitive restructuring, where you learn to challenge mind reading, catastrophizing, and all-or-nothing conclusions. The second is behavioral experiments, where you test beliefs instead of assuming they are true. The third is response delay, where you pause urges to text, check, or seek reassurance. The fourth is self-soothing and emotional regulation, so you are not asking another person to do all the calming for you. The fifth is core belief work, which addresses the deeper beliefs that keep repeating, such as “I am unlovable,” “People always leave,” or “I have to earn closeness.”

A practical CBT roadmap over the first few months
In the early phase, you usually track triggers and notice patterns. This stage feels simple, but it is not. Most anxious reactions happen fast, and many people only notice the panic after it is already running the show. So the first real win is learning to catch the moment earlier. You may keep a thought log, rate anxiety, track body sensations, and record what behavior followed the trigger.
The middle phase usually targets your interpretations. This is where you stop treating every fear as a fact. A delayed reply no longer automatically means rejection. A distracted partner no longer automatically means disinterest. You look at evidence for and against the thought, consider alternatives, and test which explanation fits reality best. Around this stage, therapists often introduce response delay and behavioral experiments, because insight without practice changes very little.
The later phase is about building secure behavior on purpose. That means saying what you need without accusation, tolerating uncertainty without chasing relief, making choices that protect self-respect, and handling closeness without fusion. Progress here is not “I never get triggered.” Progress is “I recover faster, react less impulsively, and do not let one moment define the whole relationship.” CBT is often short-term, but deeper patterns can take longer, especially when trauma or chronic instability is involved.
CBT exercises that actually help outside therapy
A thought record is one of the most useful tools because it forces your mind to slow down. You write the trigger, the first thought, the emotion, the urge, the evidence for the thought, the evidence against it, and a more balanced alternative. That sounds basic, but it exposes how often your nervous system fills in missing information with worst-case guesses. Over time, this helps reduce automatic spirals.
Another strong tool is the reassurance delay. When you want to send the fifth text, ask for another promise, or check social media for clues, you set a waiting period. It could be 10 minutes at first, then 20, then longer. During that delay, you use grounding, breathing, or a competing action like walking, journaling, or calling a friend for general support rather than relationship analysis. The point is not suppression. The point is proving you can survive uncertainty without feeding the cycle. That matters because many anxious behaviors are quick attempts to lower distress, not true solutions.
A third exercise is the secure response script. Instead of reacting from panic, you rehearse what a more secure version of you would do. That might sound like, “I noticed I feel activated. I do not have enough information yet. I will wait, regulate, and respond later if needed.” This is not fake positivity. It is disciplined realism. You are replacing fear-based interpretation with grounded language that keeps you connected to facts.
How CBT helps in real relationship situations
The hardest part of anxious attachment is that it often gets blamed entirely on the anxious partner. That is lazy thinking. Yes, your reactions are your responsibility. But context matters. A respectful, consistent partner and a vague, hot-and-cold partner do not produce the same emotional environment. CBT helps you separate your history from the current facts. Sometimes the work is calming an exaggerated fear. Sometimes the work is admitting the relationship really is unstable and your anxiety is not random.
This matters most in the classic anxious-avoidant pairing. If one person pursues and the other withdraws, each person can trigger the other. CBT helps the anxious partner stop chasing certainty through protest, panic, and overcontact. It also helps them notice whether the relationship can support healthy repair at all. Therapy should never teach you to become endlessly calm inside a bond that stays chronically inconsistent, dismissive, or emotionally unsafe. Better thinking includes clearer judgment about who you are attached to.
When CBT alone may not be enough
Some people need more than standard CBT tools. If your anxious attachment is tightly tied to trauma, severe panic, dissociation, obsessive checking, deep depression, or a history of abusive relationships, a broader treatment plan may fit better. In those cases, a therapist may combine CBT with trauma-focused work, schema therapy, DBT skills, somatic strategies, or medication management when indicated. That is not a failure of CBT. It is just good clinical judgment.
You should also be careful not to label every painful relationship issue as anxious attachment. If your partner lies, disappears, threatens breakup to control you, refuses basic accountability, or creates chaos on purpose, the answer is not only more self-regulation. The answer may include boundaries, couples therapy, or leaving. CBT should help you think more clearly, not tolerate bad treatment more quietly.
How to choose the right therapist
A therapist is not a magic fix, and picking badly wastes time. Look for someone who understands both CBT and attachment patterns, not someone who only throws around attachment language because it is popular. Ask direct questions before booking.
- Do you use CBT for relationship anxiety and reassurance-seeking patterns
- How do you handle core beliefs like abandonment, shame, or unworthiness
- Do you give homework between sessions
- How do you tell whether progress is actually happening
- What do you do if trauma, panic, or depression is part of the picture
You also want a therapist who can explain their method clearly. If they cannot describe how treatment works, that is a bad sign. CBT is structured. A decent therapist should be able to tell you what you will practice, why it matters, and how improvement is measured.
Signs CBT is working for anxious attachment
Progress rarely looks dramatic at first. It usually shows up as smaller, steadier changes. You pause before reacting. You stop checking as often. You recover faster after a trigger. You ask for needs directly instead of hinting, testing, or spiraling. You tolerate gaps in contact better. You stop treating every feeling as proof. You start noticing that your self-worth cannot stay fully outsourced to another person.
That is the real shift. Secure functioning is not emotional numbness. It is the ability to feel activated without becoming controlled by activation. Some research suggests attachment anxiety can improve during psychotherapy and CBT-linked treatment, but the lived sign of progress is practical. You feel more anchored in yourself. You can stay close without clinging and speak honestly without collapsing. That is what people are usually looking for, even when they think they are just looking for relief.
Frequently Asked Questions
Conclusion
Cognitive Behavioral Therapy for Anxious Attachment is useful because it deals with the part of the problem that shows up every day. It helps you catch distorted thoughts, reduce reassurance-driven behavior, regulate your body, and build more secure relationship habits. It does not promise instant healing, and it should not. Real change is slower than that. But it can be concrete, measurable, and durable.
The bigger truth is this. Anxious attachment improves when you stop letting fear make every relational decision. CBT helps you do that by replacing panic-based interpretation with evidence-based thinking and replacing compulsive coping with deliberate action. When that happens, relationships get clearer. So do your standards. And that is where secure attachment starts.
